Cornea Transplants/DSEK
Dr. Murray Friedberg is a fellowship-trained corneal specialist performing several cornea transplant techniques. More than 45,000 cornea transplants are performed worldwide each year with excellent success rates for many diagnoses. Surgery is usually performed on an outpatient basis, allowing the patient to go home the same day. Additional surgery may be performed at the time of corneal transplantation – cataract removal, intraocular lens implantation or replacement.
Human donor tissue is provided by an eye bank which carefully screens the tissue. Federal regulations require eye banks to screen all tissue for AIDS, Hepatitis, and a variety of other diseases. Because of the availability of corneal tissue, surgery can often be scheduled as an elective procedure at a time convenient for the patient.
As with any type of surgery, there are risks associated with corneal transplant surgery. These include infection, graft rejection, glaucoma, retinal detachment and swelling. If there are complications, additional surgery could be needed and vision could be lost.
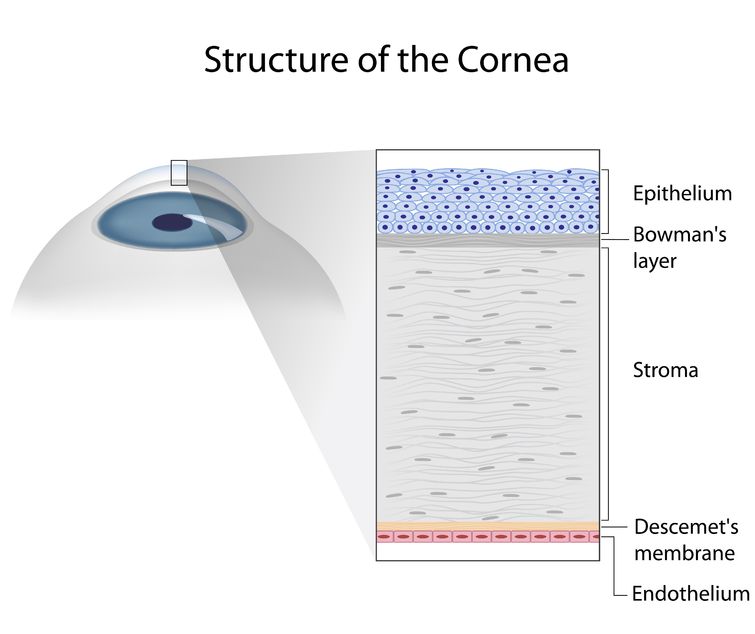
The cornea has five layers. The outermost layer is the Epithelium. A corneal abrasion occurs when this layer is injured. Bowman’s layer is just beneath the epithelium. The Stroma is the thickest central part of the cornea. Scar tissue in the Stroma can block the light going through the cornea and cause blurred vision. The innermost layer of the cornea is the Endothelium, a single layer of cells that pumps fluid out of the cornea to make it clear. This layer is attached to the stroma by Descemet’s membrane.
There are two types of cornea transplantation performed at Coastal Eye Institute: Descemet’s Stripping Endothelial Keratoplasty (DSEK) and Penetrating Keratoplasty (PKP). DSEK treats conditions involving primarily the endothelium, such as Fuchs’ dystrophy. PKP treats conditions involving primarily the stroma, such as corneal scars and keratoconus.
Descemet’s Stripping Endothelial Keratoplasty (DSEK)
DSEK is an exciting procedure that was developed more recently. DSEK is indicated when a patient only has a problem with the inner lining of the cornea, called the endothelium. Fuchs’ dystrophy is an example of such a condition. DSEK involves replacing only the damaged portion of the cornea, leaving the remaining patient’s healthy cornea behind. DSEK offers a much quicker recovery time than PKP, allowing patients to often recover in a few months rather than 6-12 months.
The picture to the right shows a DSEK graft immediately following surgery with a small air bubble to keep it in place. Rather than suturing the transplant in place, air is used to position the transplant until it permanently sticks to the patient’s inner cornea. The air bubble disappears in the first 24 -36 hours. If the graft does not continue to stay in place, sometimes an additional air bubble is needed. Descemet’s Membrane Endothelial Keratoplasty (DMEK) is an alternative to DSEK and is not performed at Coastal Eye Institute.
DSEK Surgery
Penetrating Keratoplasty (PKP)
Penetrating Keratoplasty (PKP) is a full thickness replacement of the central cornea with donor tissue. PKP is performed when the condition involves the corneal stoma and DSEK would be ineffective. Examples include keratoconus and corneal scars. Special microsurgical instruments and an operating microscope are used to remove a disc of tissue (about 8 mm in diameter) from the patient’s cornea. Donor tissue is prepared by removing a matching disc of corneal tissue from the donated human cornea.
The new cornea is secured to the patient’s eye with delicate sutures. During the first few weeks after surgery, the vision is usually blurred but progressively begins to clear. After four to six months of healing, some of the sutures may be removed to reduce astigmatism. Healing may require six to twelve months before eye glasses can be prescribed. Alternatives to PKP are eyeglasses, contact lenses, and other surgical procedures not performed at Coastal Eye Institute such as Intacs® Corneal Rings, corneal cross-linking and Deep Anterior Lamellar Keratoplasty (DALK).
